 Homocysteine levels, not cholesterol, are a critical risk factor for heart disease. Howeve, homocysteine isn’t the complete evil that it is made out to be. It is a naturally occurring amino acid that plays an important role in many aspects of good health. Chronically high homocysteine levels are the problem.
Homocysteine levels, not cholesterol, are a critical risk factor for heart disease. Howeve, homocysteine isn’t the complete evil that it is made out to be. It is a naturally occurring amino acid that plays an important role in many aspects of good health. Chronically high homocysteine levels are the problem.
The Danger of High Homocysteine Levels
High homocysteine levels indicate chronic vascular inflammation. This sets the stage for atherosclerosis (hardening of the arteries) and plaque formation that blocks blood flow. Vascular plaque leads to blood clots, heart attacks, and strokes. Fortunately, certain B-vitamins can go a long way in keeping homocysteine in check, right where it is supposed to be.
Where Do We Get Homocysteine?
All homocysteine in the body is made naturally by our own metabolism. It is derived from methionine, which is an essential amino acid found abundantly proteins from meats, seafood, dairy products, and eggs. Vegetable proteins are generally pretty low in methionine, except for certain seeds such as sesame seeds and Brazil nuts. Even legumes contain relatively small amounts of methionine compared with animal-derived protein sources.
Excess methinone is not a problem, though. Excess homocysteine is.
Once it is formed from methionine, homocysteine can do two things:
- Revert back into methionine by a process called methylation, which is aided by vitamin B12 and folic acid (also a B-vitamin).
- Convert into another amino acid, cysteine, by a process called transsulfuration, which is aided by vitamin B6.
Interconversions among methionine, homocysteine, and cysteine are crucial to good health for four main reasons:
- They enhance the production of glutathione, one of our most important natural antioxidants.
- They help the binding of minerals such as copper and zinc, thereby making them bioavailable to your body.
- They aid DNA and RNA metabolism that controls how genes are regulated.
- They guide the proper synthesis of neurotransmitters that play an important role in mood regulation.
The key point is that the formation of homocysteine is a natural process that is regulated by the presence of vitamins B6, B12 and folic acid. Normally homocysteine comes and goes quickly as it converts to either methionine or cysteine. However, if your levels of vitamins B6, B12 or folic acid are too low, these interconversions slow down and homocysteine levels build up.
How Does Homocysteine Damage Arteries?
Scientists believe that homocysteine damages arteries in at least two possible ways. One is that it induces a powerful immune reaction within the walls of arteries. Immune complexes that run amok inside artery walls cause microscopic pock marks in the innermost wall layer, the endothelium.
These rough spots in the endothelium trap substances such as calcium and small, high density LDL cholesterol particles.
That is how plaque gets started.
The other possibility is that homocysteine can damage adhesion molecules that hold endothelial cells together. When cellular adhesion is destroyed, cells can become separated, thereby forming holes or pock marks that can, once again, initiate the build up of plaque.
Once plaque gets started, it continues to grab and hold substances that normally flow freely through arteries. Keep in mind that this is how plaque builds up inside arteries. Substances that make up the plaque, however, are not the culprits that got it started in the first place. This is why the accumulation of LDL cholesterol and calcium in plaque is an after-effect, not a cause of vascular disease.
SIDENOTE: Can you imagine that, once calcium and LDL cholesterol were found to be concentrated in plaque, scientists could have flipped a coin to decide which one caused the problem? Invoking cause and effect either way is a major flaw in logic. Nevertheless, if the powers that be chose calcium, do you think we would have an entire industry based on drugs that lower calcium levels to combat heart disease? It seems ridiculous, doesn’t it? Well – surprise – it is equally ridiculous to blame cholesterol. This is why cholesterol-lowering drugs do nothing to reduce heart disease risk. Cholesterol-lowering drugs are just a great big scam.
Homocysteine Levels: How High is Too High?
Population surveys from clinical laboratories indicate a normal range of homocysteine in the blood to be 5 to 15 μmol/L. However, the associated heart disease risk increases rapidly at the upper end of this range.
This table shows how homocysteine levels correspond to cardiac risk levels:
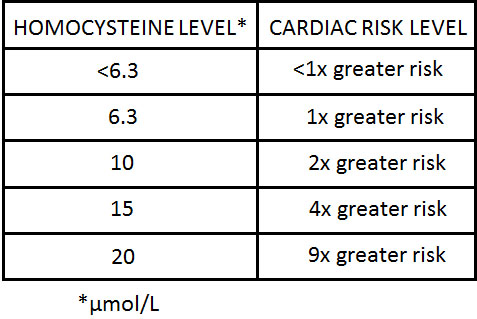
Based on these data, the recommended levels of homocysteine in blood should be less than 7-8 μmol/L.
How Can You Lower Homocysteine?
If you are thinking ahead, the obvious thing to do is supplement with those B-vitamins that regulate the interconversions among methionine, homocysteine, and cysteine. Indeed, that is exactly the best step you can take for supplementation.
Specifically, up your intake of those B-vitamins that regulate homocysteine metabolism, which are:
- Vitamin B6 – in the form of pyridoxal-5-phosphate
- Vitamin B12 – preferably as methylcobalamin
- Folic acid – as active folate, i.e., 5-MTHF (5-methyltetrahydrofolate)
Other supplements can also be helpful. These are the most crucial ones.
How Much Should You Take?
At first, this would depend on your level of homocysteine. However, a general rule of thumb is that the U.S. RDA of B-vitamins is pathetically low. Any good B-vitamin supplement will exceed the RDA by several-fold. In the case of vitamin B12 it may even be 100-fold or higher than the RDA.
When evaluating a multivitamin or B-complex supplement, make sure that your daily intake of folate is 400-800 micrograms and of vitamins B6 and B12, at least 2 milligrams each.
Indeed, in the view of many medical professionals who pay attention to the power of supplementation, the general feeling is that you cannot take enough B vitamins.
Dietary Sources of B-Vitamins
Most B-vitamins are readily available in many foods.
Folate naturally occurs in green leafy vegetables, the darker green the better. High levels are found in avocado, spinach, liver, yeast, asparagus, and Brussels sprouts. It also occurs in fruits and fruit juices, nuts, beans, peas, dairy products, poultry and meat, eggs, seafood, grains, and some beers (yay!).
Foods that contain large amounts of vitamin B6 include pork, turkey, beef, bananas, chickpeas, potatoes, and pistachios.
Regarding vitamin B12, ultimately the best food sources include most animal derived foods – fish and shellfish, meat (especially liver), poultry, and eggs. Heat destroys this vitamin, so minimizing or eliminating cooking provides the most dietary B12.
As a rule, plants rarely produce vitamin B12. Even algae that purportedly produce it actually do not do so.
By the way, vegetarians are most likely to suffer from vitamin B12 deficiency. Infants are at a higher risk if they were born to vegetarian mothers. The elderly who have diets with limited meat or animal products are also very vulnerable to B12 deficiency.
The slightly good news is that animals, including humans, can obtain small amounts of vitamin B12 from their normal gut bacteria.
Homocysteine and Aging
Note that homocysteine levels have been observed to increase with aging. This observation underlies the notion that rising homocysteine levels are normal.
This is decidedly NOT true.
It is more likely that rising homocysteine levels reflect a lifetime of chronic poor food choices, combined with a diminished ability to absorb nutrients from foods as we get older.
Making up for vitamin deficiencies by eating better is certainly helpful. It is unfortunately not sufficient without proper supplementation.
Can you tell me where I can get the reference for your homocysteine chart and Cardiac Risk?
Hi, Josiah…Thanks for your interest. Your request sent me scurrying around to find my sources for that post from more than 2 years ago. The image itself appears in two places:
http://russellwellnesscenter.com/quantum-nutrition.html
https://www.thehealthymelissa.com/the-most-important-test-for-alzheimers-stroke-heart-attack/?v=7516fd43adaa
…with additional data about nutritional support here:
https://www.patrickholford.com/advice/how-to-lower-your-homocysteine-level
None of these sources provides a journal reference. However, you can find the actual published data you seek in this 1996 article in the American Journal of Epidemiology (see Table 5) (you can download the pdf file at no charge there):
https://www.kidney-international.org/article/S0085-2538(15)48313-9/fulltext
I hope that is what you are looking for. If not, let me know.
All the best,
Dennis
Hi I am really concerned as my Plasma Homocysteine level is 30 (normal reference range is 0-15).
I have had issues with Folate deficiency for over a year. Gastroenterology found no issues with camera investigations of my gut and biopsies of colon etc..
I have also had issues with my Organic Phosphate levels – deficient.
I eat a mainly veg diet with fish & chicken occasionally.
I am concerned as no one seems to be able to get to the bottom of what is wrong.
I have suffered with Chronic fatigue for the last couple of years and recently diagnosed with a pituitary tumor which I am on medication for (bromocriptine started 15/12/19). All my hormones had fallen below the normal range and upon investigation they found a micro adenoma.
I also have primary Lymphedema in my legs and lymphatic system is sluggish in legs.
I have daily nose bleeds from my left nostril. Visual disturbance from my left eye – white lights floating up left eye. Ophthalmology could not find the cause.
I also have developed memory problems.
I have started folic acid again but when I come off it my folate drops immediately. I am taking Vit D due to being deficient. I was recommended to take Iron but got constipated.
I just feel terrible. Any advice??
Hi, Wendy…My first bit of advice is: stay positive. As challenging as that can be with so many health issues, it is the best attitude for all situations. My second bit of advice is: don’t take medical advice over the internet. The rules are against even giving such advice here in the U.S. You probably have something like that in place in the UK, too. I am doubly prohibited from advising you, since I am also not a medical doctor. With all that being said, I am confident that ALL of your challenges are based on lifestyle choices. The good news about that is, you can change them. The key is to learn what you are doing so you can biohack yourself for getting better. Since you have such a long list of issues, I’m going to give you two “reading assignments” to get started on figuring out what is going on and how to change yourself. (That’s the old professor in me, so here we go.) The first is the best health book I have ever discovered: Epi-paleo Rx: The Prescription for Disease Reversal and Optimal Health by Dr. Jack Kruse. It is widely available on the internet (e.g., Amazon). The second is Dr. Kruse’s health forum at https://forum.jackkruse.com/index.php. You can peruse it or, better yet, join it (no cost) and interact with many others who have also had seemingly intractable health problems – and revered them. (Sometimes Dr. Kruse will also peek in and provide some pointers.) His website is loaded with great information, too: https://jackkruse.com/. My third and final (for now) bit of advice is: use these information sources to get started on healing yourself ASAP. You can do it. Indeed, you are the only one who can.
All the best in natural health,
Dennis
Bless you! Thanks so much Dennis!
You are very welcome, Wendy. I’d be thrilled to know how you are doing as you figure out what changes you can make.
Cheers,
Dennis